Molina Healthcare Tech Radar: Integrating dual systems and deploying utilization management to optimize costs
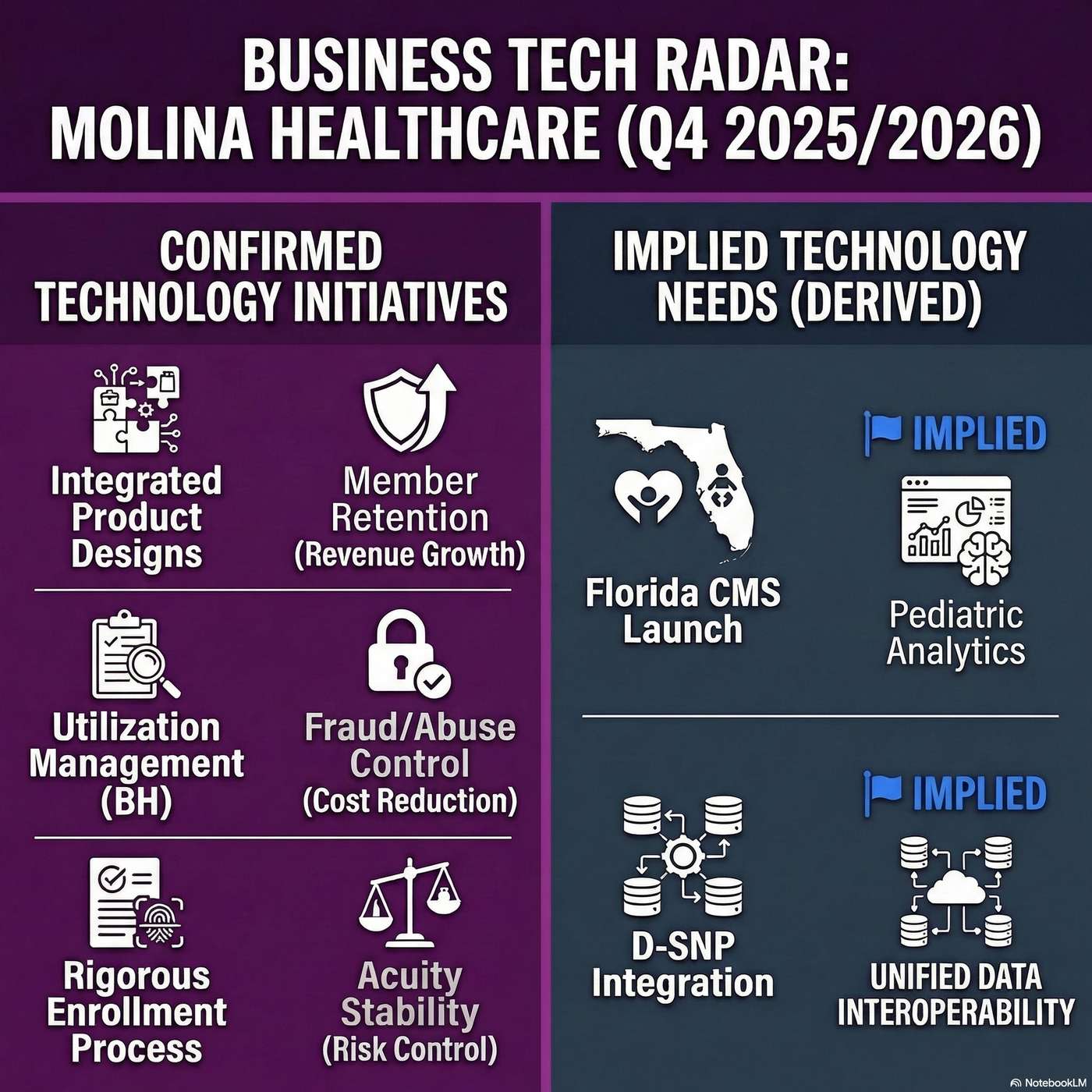
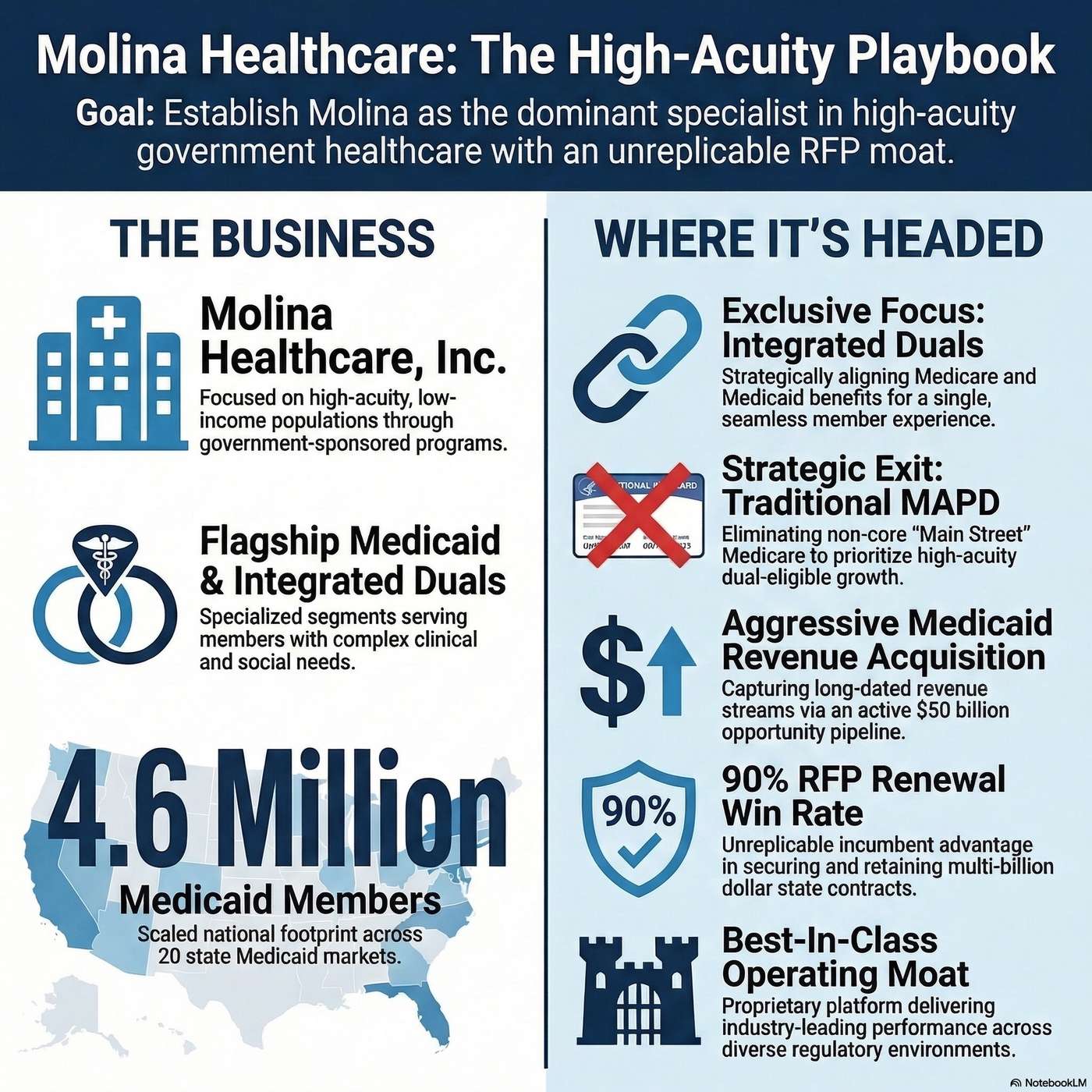
Molina Healthcare's biggest technology story revolves around aggressive cost optimization and risk management through rigorous utilization controls and the operational integration of complex dual-eligible members.
Executives explicitly confirmed rolling out stricter utilization management protocols to curb runaway pharmacy costs, specifically restricting GLP-1s to appropriate diagnoses, and managing behavioral health utilization.
They also highlighted their exhaustive data analysis of "low and no user" cohorts to model medical cost trends, and the ongoing operational prep for their $6 billion Florida Children's Medical Services contract, which requires onboarding staff to new core business systems.
Molina is undertaking a massive shift toward fully integrated duals (FIDE/HIDE programs). Because executives noted that maintaining "two membership cards, 2 call centers, 2 networks" makes no sense for a single member, Molina will logically require major technology transitions to unify siloed claims engines, provider directories, and CRM platforms.
Their strategy of acquiring struggling regional health plans at book value also implies an urgent need for rapid, repeatable post-merger IT integrations to achieve target margins.
All sourced directly from Molina Healthcare's Q4 2025 earnings call and 2026 TD Cowen conference presentation.