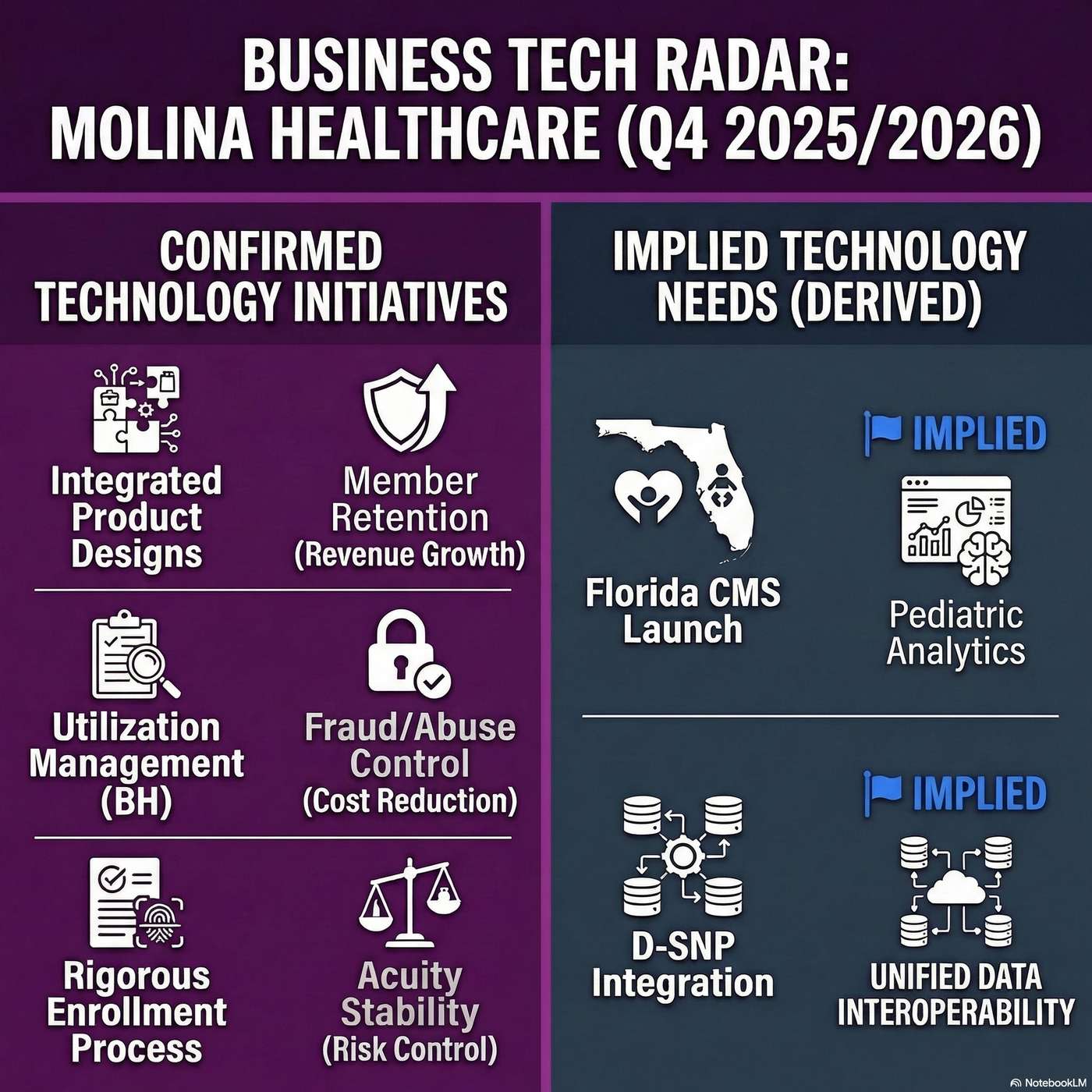
Inside Molina Healthcare: Managing government healthcare while focusing on high-acuity dual populations
Business Synopsis & Direction.
Molina Healthcare operates managed care plans focused exclusively on government-sponsored healthcare programs, primarily Medicaid, Medicare, and the ACA Marketplace.
The company generates revenue through state and federal premiums to manage member health.
Leadership is currently navigating a period of high medical cost trends by strictly focusing on profitable growth, significantly reducing volatile Marketplace exposure, and steering Medicare operations toward fully integrated dual eligible programs.
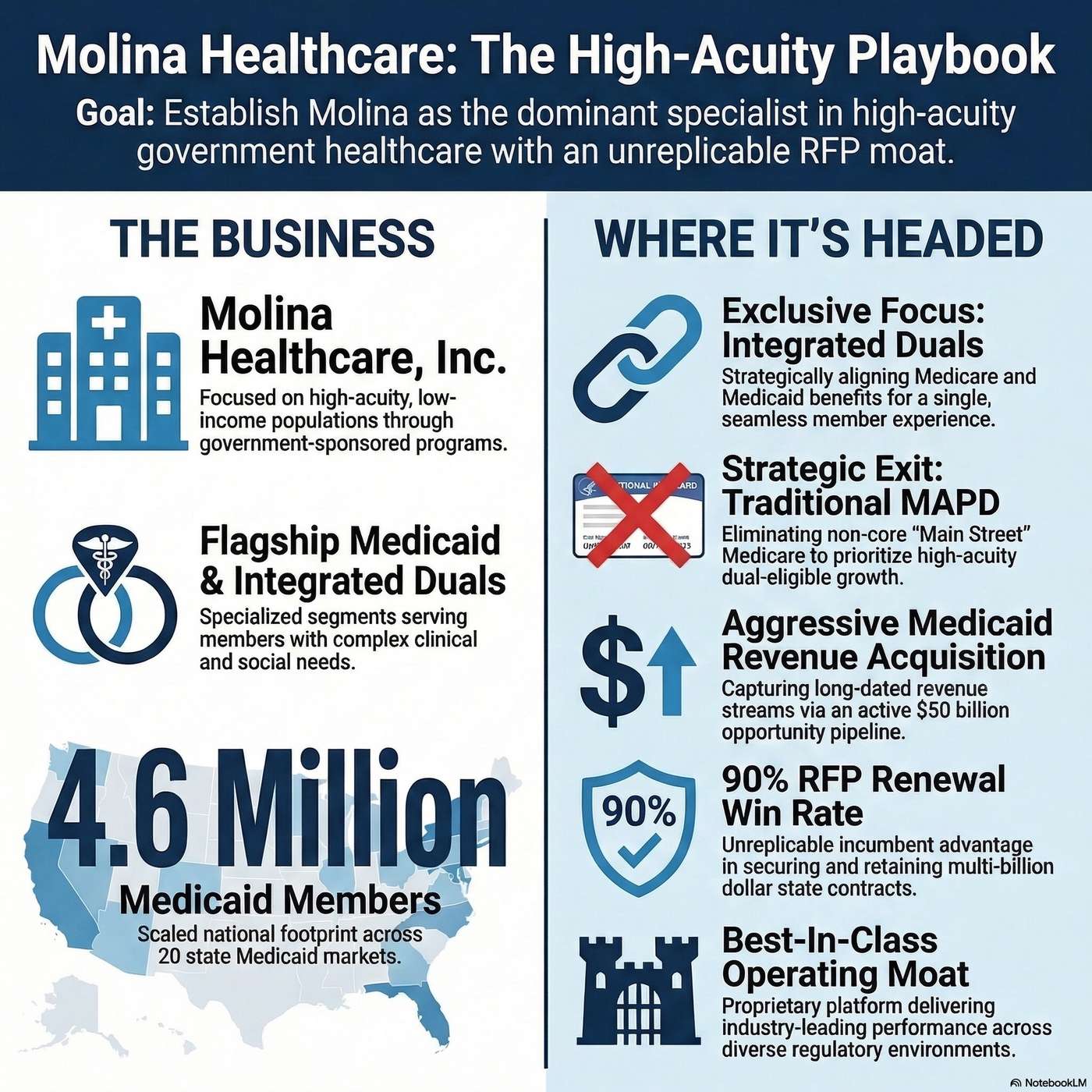
Differentiation & Products.
Molina differentiates itself through its best-in-class Medicaid cost management, typically operating 300 to 400 basis points better than the market average.
This structural advantage allows the company to remain profitable even when state rates fail to keep pace with medical trends, while competitors operate at a loss.
The company's competitive moat is its specialized expertise in managing high-acuity, low-income populations, which recently secured a historic $6 billion contract for Florida's Children's Medical Services.
Strategy & Key Priorities.
President and CEO Joe Zubretsky and CFO Mark Keim emphasize that 2026 represents a trough for Medicaid margins, with an eventual return to target margins driven by necessary state rate restorations.
They are prioritizing a strategic pivot away from traditional Medicare Advantage to exclusively focus on dual eligible members.
Management also highlighted an opportunistic M&A strategy to acquire struggling health plans at book value to secure long-dated revenue streams."All sourced directly from Molina Healthcare's own leadership from earnings calls and analyst briefings."